Understanding Eczema
Causes, Symptoms, and Management
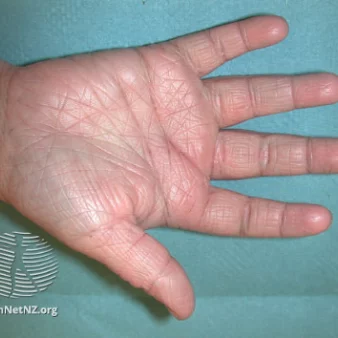
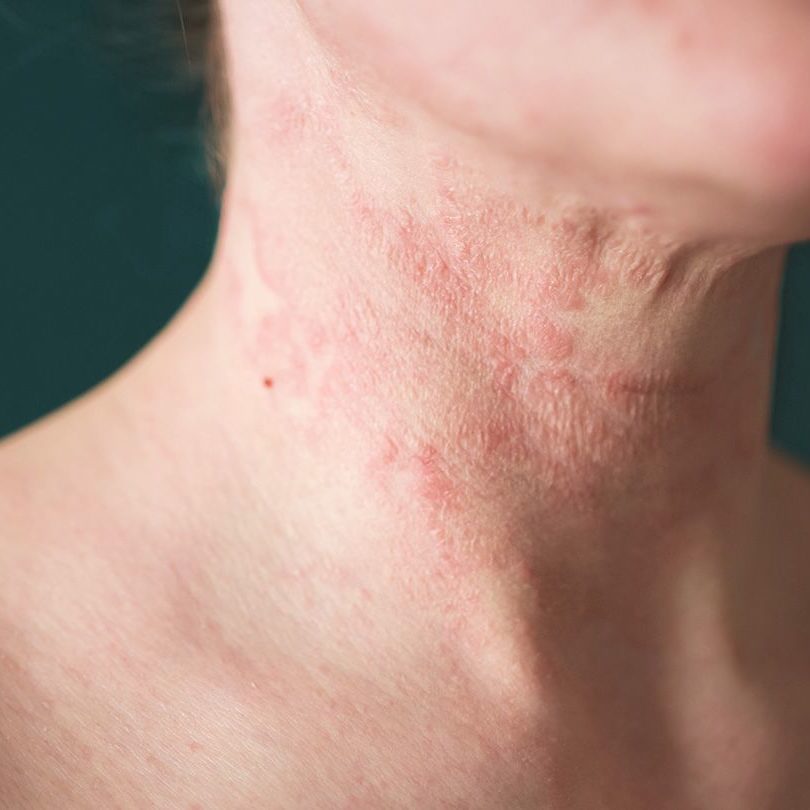
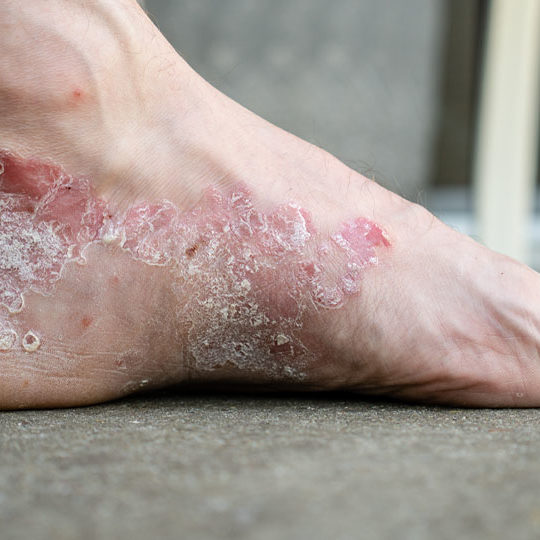
Eczema, also known as atopic dermatitis, is a chronic skin condition that affects millions of people worldwide, and can show up in multiple ways. It is characterized by dry, itchy, and inflamed skin, often accompanied by redness, rash, and occasional flare-ups. Eczema can be a frustrating and uncomfortable condition, but with the right knowledge and management strategies, individuals can effectively control and minimize its impact on their lives.
Causes of Eczema:
1. Genetic Factors: Research suggests a strong genetic predisposition to eczema. According to the American Academy of Dermatology (AAD), specific gene variations impact the skin's ability to retain moisture and protect against irritants, making individuals more susceptible to developing eczema. Moreover, having a family history of allergies, asthma, or eczema increases the risk of developing the condition.
2. Immune System Dysfunction: The immune system plays a significant role in eczema development. The AAD explains that individuals with eczema have an overactive immune system, which reacts excessively to triggers, leading to inflammation in the skin. This abnormal immune response manifests as redness, itching, and swelling – classic symptoms of eczema.
3. Skin Barrier Dysfunction: The skin's outermost layer, known as the epidermal barrier, acts as a protective shield against external irritants and allergens. In individuals with eczema, this barrier is compromised, allowing irritants to penetrate more easily. Moisture loss occurs, resulting in dryness, which further exacerbates the condition.
Triggers of Eczema:
1. Allergens: The AAD highlights common allergens as potential triggers for eczema flare-ups. These include pet dander, dust mites, pollen, certain foods, and mold. Identifying and avoiding these allergens can help minimize symptoms and prevent exacerbations.
2. Irritants: Contact with irritants can trigger or worsen eczema symptoms. The AAD advises individuals with eczema to avoid harsh soaps, detergents, fragrances, certain fabrics (like wool or synthetic fibers), and chemicals found in personal care products to reduce the likelihood of irritation.
3. Dry Skin: Dry skin is a well-known trigger for eczema. The AAD emphasizes that when the skin lacks proper moisture, it becomes more susceptible to irritation and inflammation. Regular moisturization is vital in managing and preventing eczema symptoms.
4. Climate and Temperature Changes: Environmental factors, such as extreme weather conditions, can trigger eczema flare-ups. The AAD notes that cold, dry winters or hot, humid summers can disrupt the skin's moisture balance, leading to increased susceptibility to eczema symptoms. Rapid temperature changes, excessive sweating, and exposure to dry air should be taken into consideration.
5. Stress: Emotional stress has been recognized as a potential trigger for eczema. The AAD explains that stress can weaken the immune system and contribute to flare-ups. Managing stress through techniques like meditation, exercise, and relaxation exercises may help reduce the frequency and severity of eczema symptoms.
6. Hormonal Changes: Hormonal fluctuations, particularly in women, can influence eczema symptoms. The AAD highlights that hormonal changes during puberty, pregnancy, and menopause can lead to eczema flare-ups. Understanding and managing these triggers can aid individuals in effectively controlling their condition during these periods.
Common Symptoms of Eczema:
1. Itching: Itching is a hallmark symptom of eczema and is often intense and persistent. The AAD notes that itching can become particularly severe during flare-ups and can significantly impact a person's quality of life.
2. Redness and Inflammation: Eczema-affected skin typically appears red and inflamed. The AAD explains that this is due to increased blood flow and inflammation in the affected areas. The redness may be patchy or diffuse, depending on the severity of the condition.
3. Dry, Scaly Skin: Dryness is a common feature of eczema. The AAD emphasizes that individuals with eczema often experience excessive dryness, resulting in rough, scaly skin. The affected areas may feel rough to the touch and appear flaky.
4. Rash or Eruptions: Eczema can manifest as raised patches of skin or rashes. According to the AAD, these rashes may vary in appearance and can range from small, red bumps to larger, raised plaques. In some cases, the rashes may develop fluid-filled blisters that can ooze or crust over.
5. Cracked Skin: As eczema progresses, the skin can become increasingly dry and cracked. The AAD highlights that the cracks may be superficial or deeper, leading to potential pain and discomfort. Cracked skin can also make the affected areas more susceptible to infections.
6. Thickened, Lichenified Skin: In chronic cases of eczema, the skin can become thickened and lichenified. Lichenification refers to the skin becoming thick, rough, and hardened due to persistent scratching or rubbing. The AAD explains that this thickened skin may be darker in color than the surrounding skin.
7. Secondary Infections: Continuous scratching and breaks in the skin barrier can make individuals with eczema more prone to secondary bacterial or viral infections. The AAD advises seeking medical attention if signs of infection, such as increased redness, pain, warmth, or pus, develop.
Management and Treatment
1. Moisturize Regularly: Moisturizing is a fundamental aspect of eczema management. The AAD emphasizes the importance of applying moisturizers multiple times a day, especially after bathing, to lock in moisture and prevent dryness. Opt for fragrance-free, hypoallergenic moisturizers that are gentle on the skin. Thick ointments or creams are usually more effective than lotions.
2. Identify and Avoid Triggers: Identifying and avoiding triggers can help minimize eczema flare-ups. The AAD suggests keeping a journal to track potential triggers such as specific foods, fabrics, soaps, detergents, or environmental allergens. Once triggers are identified, take proactive steps to avoid or minimize exposure to them.
3. Adopt a Gentle Skincare Routine: Developing a gentle skincare routine is crucial for individuals with eczema. The AAD recommends using mild, fragrance-free cleansers and avoiding hot showers or baths, as they can strip the skin of moisture. Gently pat the skin dry with a soft towel and avoid vigorous rubbing, which can worsen irritation.
4. Topical Medications: Topical medications are commonly prescribed for managing eczema symptoms. According to the AAD, over-the-counter or prescription corticosteroid creams or ointments can effectively reduce inflammation and itching during flare-ups. Non-steroidal options, such as calcineurin inhibitors, may also be recommended for long-term management. It is essential to follow the prescribed usage instructions and consult a dermatologist for guidance.
5. Antihistamines: Antihistamines may be recommended to alleviate itching and promote better sleep during eczema flare-ups. The AAD suggests discussing with a healthcare professional to determine the appropriate antihistamine medication and dosage for individual needs.
6. Wet Wrap Therapy: Wet wrap therapy can provide soothing relief for individuals with severe eczema. The AAD explains that this technique involves applying moisturizers and medications to the skin, followed by a damp layer and a dry layer of clothing. Wet wraps help retain moisture, enhance the absorption of topical medications, and provide a cooling effect on the skin.
7. Stress Management: Stress can exacerbate eczema symptoms. The AAD recommends practicing stress-reduction techniques such as meditation, yoga, deep breathing exercises, or engaging in activities that promote relaxation. Seeking support from mental health professionals or support groups can also be beneficial.
To get the best treatment for eczema relief, please make an appointment and see a licensed OnSpot provider.
